
Two families say they will take legal action over Do Not Attempt Resuscitation (DNAR) orders made on their loved ones at QEQM Hospital in Margate.
Birchington construction worker Terry Bolton and Whitstable businessman Alan Barker plan to challenge the decisions and the reasons behind them.
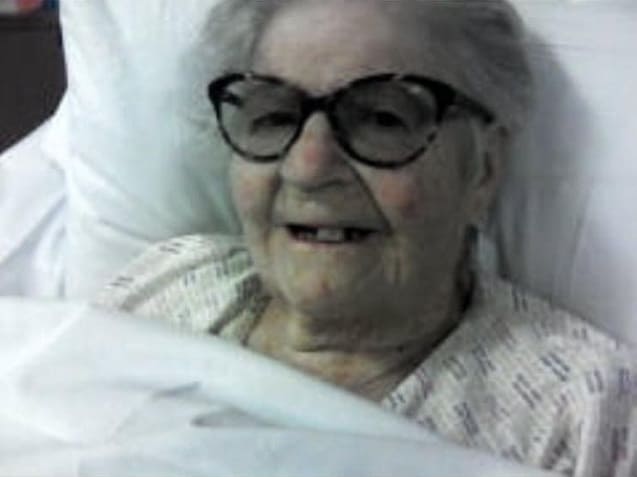
Terry’s mum Carol was being treated as end of life for a month, with the family believing she would die due to Covid after being told her organs were ‘breaking down’.
Carol defied those predictions and is now recovering in Kent & Canterbury Hospital.
- Read about Carol here: Family’s shock over ‘end of life’ decision on mum suffering covid – who then sat up and asked for cuppa
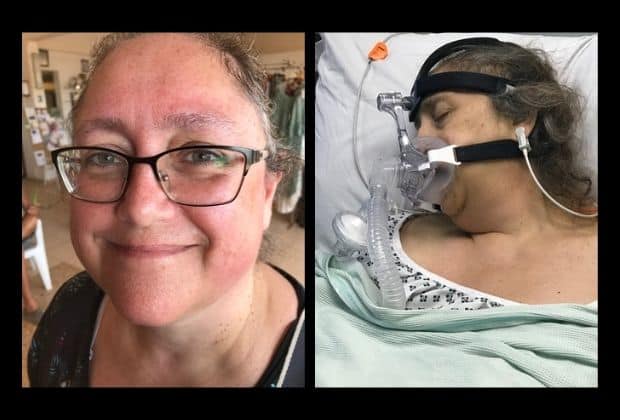
Alan says the order made on his wife Lorraine, who sadly died on Christmas Eve, was a breach of her rights and he has sought legal advice.
He complained to the hospital trust about pressure placed on the family over applying a DNAR decision.
- Read about Alan and Lorraine here: Devastated husband’s call for answers over wife’s covid contraction, do not resuscitate ‘order’ and death at QEQM Hospital
Both men have now made official requests for access to the medical files of their loved ones and Alan says he is taking specialist advice to bring a case.
Several other Thanet residents have raised concerns over use of the orders.
One woman says she is in the process of legal action over her mum’s death and another says she was treated for Covid and, after her discharge, was distressed to find a DNAR had been placed on her records without her knowledge.
‘Sensitively and honestly’
East Kent Hospitals Trust, which is responsible for sites including QEQM, says a decision not to attempt resuscitation is never taken lightly.
The Trust added that discussions and support are offered to patients and their families where possible to ensure all questions and other issues can be addressed sensitively and honestly.
A spokesperson said: “In situations where a person’s clinical condition is deteriorating despite medical treatment, it is not always appropriate to attempt resuscitation if their heart or breathing stops because the outcome of any attempt at resuscitation would not be successful at that time.
“A decision not to attempt to resuscitation is never taken lightly and discussions and support are offered to patients and their families where possible to ensure all questions and other issues can be addressed sensitively and honestly.
“The outcome of any discussions with the patient and all of the clinical information is then recorded in the patient’s notes to ensure everyone involved in the patient’s care is fully aware of the situation.”
In 2018 a Care Quality Commission report said areas for improvement at East Kent Hospitals Trust included ensuring “that consent to care and treatment is always sought in line with legislation” in regards to DNARs.
In 2015 the trust admitted breaching the human rights of a 51-year-old man after two DNACPR (Do Not Attempt Cardiopulmonary Resuscitation) orders were placed on his records in 2011, giving his disability of Down’s syndrome as one reason, without the knowledge of his family.
Court findings on DNR process
A court judgement in 2014 over the process of DNAR/ DNACPR use in hospitals found that staff must consult patients unless the clinician believes the distress caused by the discussion will harm the patient.
In those cases they must document their reasons and take reasonable steps to involve the patient’s family in the discussions. But the law does not require a patient or their family to consent to a DNAR order. A doctor can issue an order, even if the family do not want one, if medical evidence necessitates.
Health watchdog DNAR national review
The Care Quality Commission (CQC) is carrying out a national review into the application of DNACPR decisions during the Covid-19 pandemic.
Early findings show that while there is no evidence to suggest blanket approaches to DNACPR decisions, people told CQC that early in the pandemic they or their loved ones received DNACPR decisions which were not based on their wishes and needs, and without their knowledge and consent.
The CQC review continues, with the results due to be published in the early part of this year.
Rosie Benneyworth, Chief Inspector of Primary Medical Services and Integrated Care at the Care Quality Commission, said: “It is unacceptable for clinical decisions – decisions which could dictate whether someone’s loved one gets the right care when they need it most – to be applied in a blanket approach to any group of people.
“Sadly, in the experiences that people have generously shared with us there is very real concern that decisions were made which not only overlooked the wishes of the people they affected, but may have been made without their knowledge or consent.
“As we warned in our recent State of Care report, these findings highlight that inequalities in the care people receive risk being magnified by the impact of the coronavirus pandemic. As this is such an important and sensitive issue, we have worked quickly to share the interim findings and we will continue this work so that we build on the evidence already shared and can make recommendations for the future.
“It is vital that we look at what happened on the ground, continue to speak to people using services and people working in them, so that we can make sure that the health and care system learns the crucial lessons it needs to from this difficult time.
“We have also highlighted the fact that it is possible in some cases that inappropriate DNACPRs remain in place – and made it clear that all care providers have a responsibility to assure themselves that any DNACPR decisions have been made appropriately, in discussion with the person and in line with legal requirements.”

