
Military support will be used to create asymptomatic testing sites in Thanet and Swale.
The programme is to be rolled out in areas of high prevalence in Kent in the coming weeks.
This helps to identify those people who may have the coronavirus without symptoms and who are therefore potentially spreading it unknowingly within their families and local communities.
The first asymptomatic testing sites have been identified for Swale and Thanet due to the current high prevalence in those areas, and further sites are being investigated in other districts.
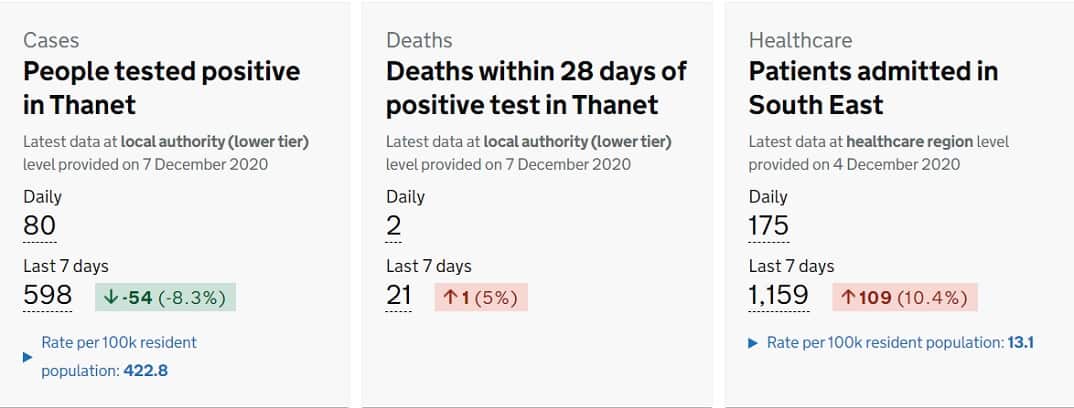
Weekly cases per 100,000 people for Thanet stands at 422.8 for the seven days to December 2, according to the government coronavirus map. The England average is 147.8.
Medway currently has the highest rates in the country at 602.8 per 100,000 according to government data.
Eighty positive tests have been reported for Thanet for today, making a total of 598 for the last 7 days – a drop of 8.3%.
Two deaths within 28 days of a positive covid death have been reported today, making 21 in the last 7 days and a total of 180 losses (within 28 days of a positive test) up to December 6.
The latest R (reproduction) number for the healthcare region of South East is estimated at 0.9 to 1.1. R is the number of people that one infected person will pass the virus to.
Lateral flow testing will help to reduce case numbers in those areas and get back to manageable levels of the virus, and place Kent in a better position to move out of Tier 3.
People without symptoms of COVID-19 will be invited to these sites, for a lateral flow test. This is a swab test, but unlike PCR where a laboratory and specialist equipment is needed, the result is given within 30 minutes. KCC will be launching a recruitment drive to run the testing sites, along with redeploying existing workforce where possible.
The Government has also already begun lateral flow testing in settings that are most vulnerable – for example care homes and NHS – across Kent.
This testing is being funded by central Government to support local councils to manage the second wave of the pandemic.

Andrew Scott-Clark, Director of Public Health said: “I need to highlight the scale of the challenge. For a county as big as Kent this is a huge undertaking. We need to have sites secured and made Covid-safe, resources recruited and trained to carry out the testing, and a robust logistical plan to ensure the storage, transportation and availability of equipment, testing kits and IT infrastructure at each site.
“We want you to understand the scope of the work we are doing and see first hand the progress we have made in a short space of time.
“KCC, District and Borough Council partners and other multi agency partners are simultaneously working on targeted asymptomatic testing, planning vaccination sites alongside the NHS, and preparing for Transition on 31st December. Our aim is to keep people as safe as we can throughout the pandemic, as well as keeping Kent moving and open for business as Transition approaches at the end of the year.
“I want to take this opportunity to thank everyone who has been working so hard this past year, your efforts are really appreciated.”
The lateral flow testing is purely for people who don’t have symptoms of coronavirus. There are tests available across the county if you have symptoms which can be booked at www.gov.uk/get-coronavirus-test
In most cases you will be able to get a test either the same day or the following day.
Hospital data
Data from East Kent Hospitals (via NHS England) shows there are 121 occupied Covid beds as of December 1 at the main sites (Margate, Ashford and Canterbury). This is down from 173 on November 30. Of those 16 mechanical ventilation beds are in use, down one from November 30. East Kent Hospitals Trust has recorded 563 covid related deaths (see footnote).
Kent and Medway Clinical Commissioning Group says: “All hospitals across Kent and Medway continue to be under significant pressure due to the high rates of infection in the local communities.
“We have opened more critical care beds to support Covid-19 patients, and will be opening more. We’re continuing to provide cancer and other urgent operations. However, we are now pausing non-urgent elective services. This will allow staff to move to support the increased number of Covid-19 patients.
“Initially this will be for a two week period. We will keep this under weekly review and will contact individual patients where appointments need to be rescheduled.
“Reports in the media that some intensive care units are full are misleading. The numbers of patients in intensive care can change on a daily or hourly basis and all hospitals are working together to make sure the most seriously ill patients are cared for. If a unit is using all of its beds at any given time we have systems in place to transfer or redirect patients.”
Military support

Since March 18, the MOD has responded to 255 COVID-19 Military Aid to Civilian Authority (MACA) requests. As of December 4, there were 2,938 military personnel committed to assist with 56 open MACA requests. This number is kept under constant review and military personnel will be available to support where needed. There are an additional 14,000 personnel on standby as part of the Winter Preparedness Package who can be called upon for COVID-19 tasks.
Local authorities that fall into tier 3 are able to apply for support from NHS Test and Trace and the Armed Forces to deliver a six-week rapid community testing programme.
This includes access to lateral flow tests and planning, logistics, funding and communications support.
Vaccination

The NHS will begin vaccinating patients against coronavirus at dozens of hospital hubs from tomorrow (December 8).
People aged 80 and over as well as care home workers will be first to receive the jab, along with NHS workers who are at higher risk.
There are 50 hubs in the first wave – including the William Harvey Hospital in Ashford – and more hospitals will start vaccinating over the coming weeks and months as the programme expands.
Patients aged 80 and above who are already attending hospital as an outpatient, and those who are being discharged home after a hospital stay, will be among the first to receive the life-saving jab.
Hospitals will also begin inviting over 80s in for a jab and work with care home providers to book their staff in to vaccination clinics.
Any appointments not used for these groups will be used for healthcare workers who are at highest risk of serious illness from covid. All those vaccinated will need a booster jab 21 days later.
GPs and other primary care staff are also being put on standby to start delivering the jab. A small number of GP-led primary care networks will begin doing so week beginning 14 December with more practices in more parts of the country joining in on a phased basis during December and in the coming months.
Susan Acott, Chief Executive of East Kent Hospitals said: “We are proud to be one of the first hospitals to begin vaccinating against Covid-19. Our staff are working extremely hard to get ready for this historic moment and we are privileged to be able play a part.
“We will be in touch directly with eligible patients and only those contacted directly should attend the hospital for a vaccination.”
Details of Covid attributed deaths data: NHS England and NHS Improvement publish the number of patients who have died in hospital and tested positive for COVID-19 in England. Since Tuesday 28 April, NHS England and NHS Improvement also reports the number of patient deaths where there has been no COVID-19 positive test result, but where COVID-19 is documented as a direct or underlying cause of death on part 1 or part 2 of the death certification process. This change has been introduced for deaths that occurred on 24 April and subsequently.
This means the NHS England and NHS Improvement data collection provides information on all COVID related (suspected and confirmed) deaths in England hospitals.

