
Care homes in Kent are struggling to get staff and residents tested for Covid-19 because swabs don’t turn up or those that do are not collected for transport to the laboratory, says Kent County Council.
In a document looking at the situation in the county’s care homes it says a local distribution hub, similar to the one run for personal protective equipment (PPE) access is needed for the Covid tests.
The document also highlight how many care homes are excluded from the process, saying: “The portal is only accessible to older people homes with dementia – no coverage for our learning disability, physical disability or mental health homes (roughly one-quarter of our WK homes have no access).
“Portal state delivery will happen and they don’t arrive on the specified days. Homes then spend days chasing and chasing often to no avail. Issues with ID numbers to log the swabs and the website to upload often isn’t working properly or isn’t easy to navigate.
“Couriers don’t always collect meaning tests are wasted and residents/staff have to go through unnecessary repeat testing – that’s if and when the home can get more swabs delivered.”
On May 25, the most recent data available, the Office for National Statistics reported 255 deaths in care homes in Kent for which Covid-19 is listed on the death certificate. Kent County Council has 543 care homes. There are around 50 in Thanet.
More than 120 care homes in Kent report continued problems getting protective clothing. Last week, almost half of all care homes were reporting that there was no testing of residents discharged from hospital into their care and 138 homes say staff work in more than one care home, and 135 homes are unable to isolate infected residents.

Kent County Council Lib Dem councillor Trudy Dean has highlighted the issue facing care home staff and residents, calling the findings ‘shocking.’
She said: “On March 17, Simon Stevens, NHS Chief Executive, instructed all hospitals to urgently discharge patients to care homes. Patients were discharged in a rush without routine testing taking place to check if they were still infected. Many care homes refused to admit discharged hospital clients, but many others felt obliged to do so.
“There do not appear to have been any step-down beds provided in Kent, as there are elsewhere, so that discharged patients could be quarantined until they were proved free of infection.
“Over two-thirds of Kent care homes have still not been able to get swab tests to identify infected staff and residents quickly. Homes report that the Government on-line portal to order tests often doesn’t work, swab tests do not arrive or are not collected, and there are delays in getting results. There are only two mobile testing units for the whole of Kent and Medway carrying out tests in areas of high demand, such as at care homes.
“These failings in the testing system mean that the spread of infection is not being stopped as quickly as possible, especially as care home staff need regular testing to ensure they remain free of the disease as they move between patients, other care homes and their own residences.
“It also probably means Covid-19 deaths in care homes are in reality being under-reported. GPs may be reluctant to identify Coronavirus as a cause of death unless a positive test has been carried out, especially as in some cases GPs have followed advice not to enter care homes.
“In the face of all these problems reported direct from the front line only last week, the Government’s claim to have put their arms around care homes from the start seems very hollow indeed.
“Now the Government has passed responsibility for preventing and controlling the spread of Covid-19 in Kent’s care homes to the county council. But until the Government gets a grip on testing and tracing and PPE supplies, there is little more that KCC can do.”
Thanet
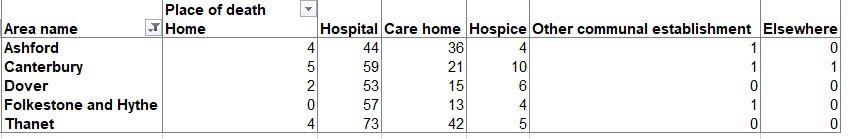
In Thanet, deaths occurring up to May 22 but registered up to May 30, show the isle suffered 124 losses with Covid cited on the death certificate. Forty-two of these were registered by care homes, 73 in hospitals, four at a private residence and five at the hospice.
County councillor Karen Constantine said most in the Ramsgate area appear to be getting the tests and PPE. She said: “I telephoned the care homes in my division to speak to the managers and they have largely reported that they are getting tests and PPE. I found a couple of homes that weren’t and I wrote to Wilf Williams, Accountable Officer for Kent & Medway CCG on Wednesday, June 3.
“Two homes have reported to me that their staff cannot obtain tests as they are not eligible. They also state that they would wish to have access to tests.
“Given Public Health England’s recent reports that nursing auxiliaries and associates are one of three occupations with significantly higher deaths at 2.5 times normal, and that people with learning disabilities are reporting death rates three times higher than 2019, I have asked him to explain why these homes aren’t able to obtain staff tests. It seems vital to me.”
County
Kent has the highest number of registered care home beds in England, with a total of 14,579 as at May 2020. There are 544 care homes registered with the Care Quality Commission in Kent, as at March 2020.
The council currently supports 4,838 people in care homes on a permanent basis including out of county placements and, commissions through contracts approximately 33% of care home beds.
It is estimated that self-funders occupy around 40% of care home beds in the county. A proportion of Kent bed capacity is occupied by other local authority placements in care homes in the county, specifically London Boroughs and Medway Council.
Supplies of PPE worth over £3.2m have been sourced and underwritten by KCC so far. Working closely with the Kent Resilience Form, this service has now delivered over 4.4million items of PPE, including 800,000 face masks, in over 2,300 separate deliveries. Over half of the care homes and homecare providers in Kent have been recipients.
A letter to government from Kent County Council and the Kent & Medway Clinical Commissioning Group says: “We have found that support from MHCLG/DHSC has been erratic and unpredictable with the council having to cover significant gaps in supply.”
Care providers in the county have come under financial pressures as elsewhere. KCC stepped in by making two payments totalling £13.5 million, to all residential, nursing, homecare and supported living and supporting independence providers.
The authority says its work has come at significant cost and it is hoped there will be more government funding forthcoming.
National picture
Government data from the ONS for deaths of care home residents attributed to Covid shows a decrease across the country to 32.5 per cent in the week to May 22, compared with 37.2 per cent in the previous week.
Cllr Ian Hudspeth, Chairman of the Local Government Association’s Community Wellbeing Board, said: “Every death from this dreadful disease is a personal tragedy and our thoughts go out to those family and friends in mourning.
“Social care is on the frontline in the fight against coronavirus. We are thankfully seeing a week-on-week decline in the number of care home deaths attributable to COVID-19, but worryingly the total number of excess deaths in care homes is still higher than the five-year average, which means our elderly and most vulnerable continue to be at risk.
“Councils are doing all they can to protect those in care homes, as well as those receiving care in their own homes. Every council in England has prepared plans on how to support all care homes in their areas to control and prevent future infection outbreaks, working alongside the NHS locally and with Public Health England.
“These plans, alongside greater information sharing with councils on where outbreaks are happening more widely as part of the test and trace programme, will help in our shared national effort to finally defeat this disease.”

