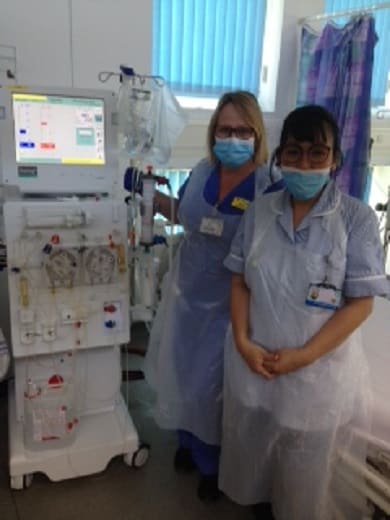
Dozens of clinical staff across East Kent Hospitals have volunteered to work in critical care units at the William Harvey Hospital in Ashford, Kent and Canterbury Hospital and Queen Elizabeth The Queen Mother Hospital in Margate during the coronavirus pandemic.
Corporate staff have moved to support frontline teams and staff working in departments such as ophthalmology (pictured below), where there are now fewer patients than usual, have volunteered for roles ranging from answering the phones on wards to cleaning.
Trust key workers are pitching in across all areas, although there are around 300 staff- about 4.5 per cent of the 8,000 staffing total – who are absent due to Covid-19 issues.
Currently East Kent hospitals still have good capacity for coronavirus patients and the Kent & Medway Clinical Commissioning Group says latest planning assumptions are that social distancing is having a positive impact on pushing back and lowering the infection rate.
Chief operating officer Lee Martin (pictured below) said: “Colleagues across all our hospitals and all our departments have been fantastic in rising to the challenge the coronavirus outbreak presents us with and working in different ways to help and support our patients.

“We have been truly humbled by their enthusiasm and dedication – both from those stepping forward to volunteer for different roles and those who welcome them with open arms and take the time to guide and support them.”
Staff who would normally be supporting the Trust in departments such as human resources, IT, information and finance, have taken over the day-to-day distribution of personal protective equipment (PPE).
Angeline Newbery, from the Trust’s improvement and transformation team, is one of those in charge of making sure the stores are open from 8am to 8pm seven days a week, managing the redeployed staff.
They work with wards to keep a log of the equipment available and bring additional supplies if stock levels drop.
Chief analytical officer Marc Farr, who has provided staff to the PPE team while he has taken on a cleaning role, said: “It’s a great way for us all to keep fit. Our usual roles mean we are sitting for lengths of time, so many of us are now measuring our steps and are walking six to 10 kilometres a day.

“The mood in the team has been very positive, people are making new connections and feel proud to be part of a team supporting our clinical frontline colleagues.”

However, the supply of PPE to the Trust has been “inconsistent in time and volume and variable in terms of content,” says chief executive Susan Acott (pictured).
She admits getting PPE out to the organisation is a daily challenge which necessitates mutual aid between organisations, and sourcing from different suppliers.
The Trust has not run out of PPE but staff are having to use it under Public Health England guidelines, which has been criticised for advising some equipment can be used for a full session rather than changed between patients.
PHE guidance
The guidelines say anyone coming within two metres of a patient with possible or confirmed case of coronavirus (Covid-19) should have kit including a fluid-resistant (Type IIR) surgical mask; plastic apron; eye protection; and gloves.
The guidance adds that PPE, namely facemasks and eye protectors, do not need to be exchanged between each patient contact, but can be used for a full session.
Royal College of Nursing
The Royal College of Nursing has raised concerns about this, saying results from a survey it carried out show of those treating possible or confirmed COVID-19 patients in high-risk areas, around half (51%) reported they are being asked to re-use items of PPE that are marked ‘single use’ by manufacturers. Of those treating COVID-19 patients elsewhere, over a third (39%) said they were being asked to re-use this equipment.
RCN Chief Executive and General Secretary, Dame Donna Kinnair, said: “This guidance was developed without full and formal consultation with the Royal College of Nursing. It is unacceptable that any healthcare setting in the UK does not provide PPE as required by HSE and set out in the existing guidance. Only sound scientific evidence or safety concerns should change the guidance. We have written to the HSE in the strongest terms to voice our concerns. Nursing staff need to be afforded proper protection full stop.”
Ms Acott said although staff are understandably anxious and want the highest level PPE they can have, Trust supply only permits it to ”issue what people need” under the PHE guidelines.
Health and Safety Executive
In a government statement, the Health and Safety Executive says: “Some of the PPE in the NHS COVID-19 Ensemble is designated by the manufacturers as being single use.
“However, the HSE recognises that some compromise is needed to optimise the supply of PPE in times of extreme shortages. It has agreed that the use (as outlined in its document) is appropriate within health and safety legislation and provides appropriate protection for health and care workers.
“These are exceptional circumstances and do not reflect HSE’s standard approach. HSE expects Trusts to have an agreed action plan to support implementation which includes a consideration of all measures to manage usage effectively.”

Last week the Secretary of State for Health and Social Care Matt Hancock said: “Global demand for this equipment is at unprecedented levels and several countries have placed export bans on the sale of PPE.
“While we entered the crisis with a stockpile designed to respond to an outbreak of pandemic influenza and a no-deal Brexit, our supply chain for PPE was designed to accommodate delivering to 226 NHS trusts.
“We are now providing essential PPE supplies to 58,000 different providers including care homes, GP surgeries, hospices and community care organisations. We also went into this crisis without a large-scale domestic PPE manufacturing industry to draw on.”
The government says it is working to ‘ramp up’ national PPE distribution.

